A 45-year-old woman presents to her GP surgery with palpitations. On examination, her heart rate is 156 bpm with an irregularly irregular rhythm. She denies chest pain or dizziness and her BP is 110/75 mmHg. She is otherwise well and has no past medical history of note. The practice nurse performs an ECG, which is shown below:
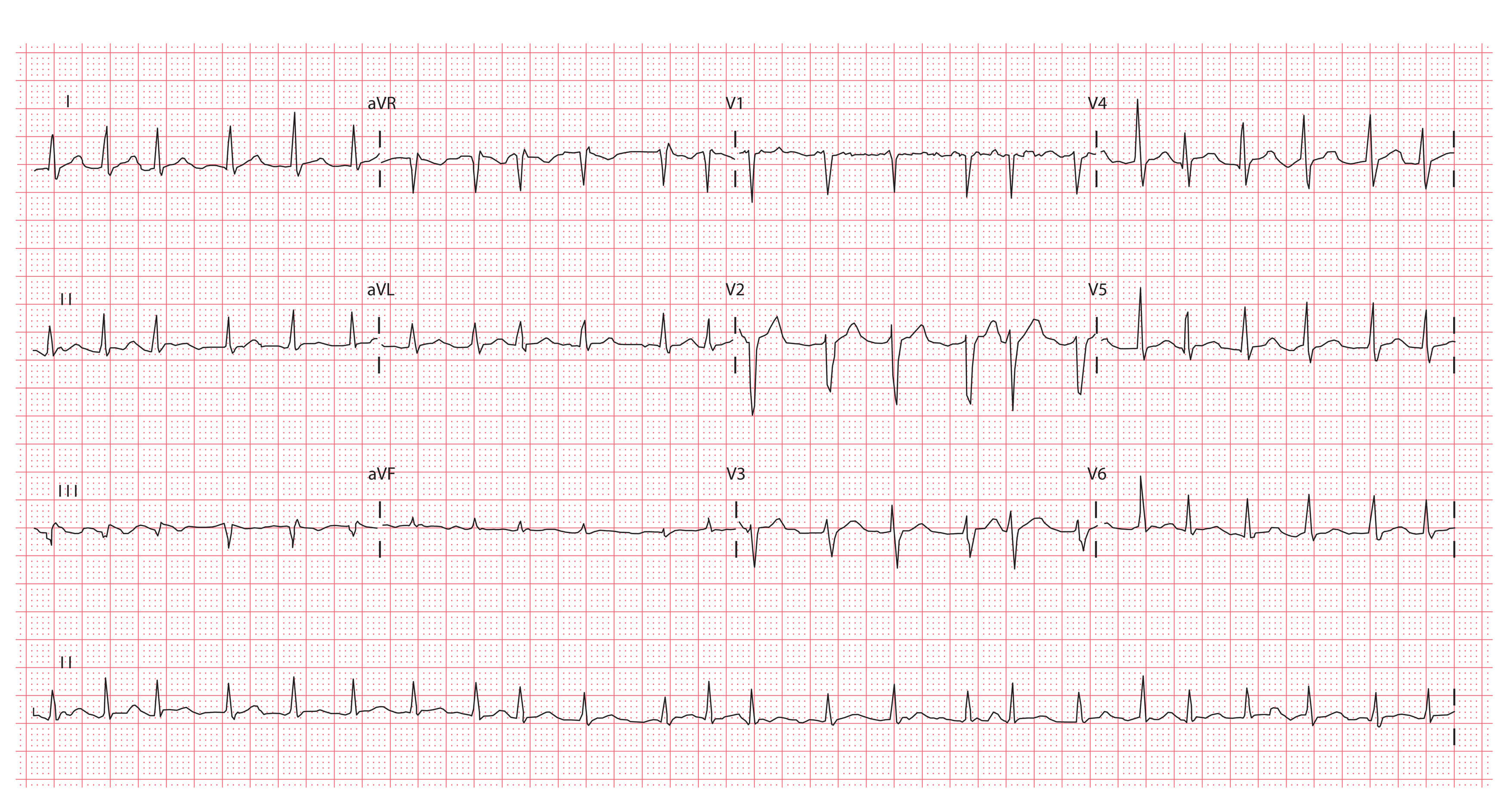
- What is the most likely diagnosis in this case?
Show Answer
This patient’s clinical features and ECG confirm a diagnosis of atrial fibrillation.
- What supporting evidence for this diagnosis is provided by the ECG in this case?
Show Answer
The key ECG features of atrial fibrillation present in this case are:
- Irregularly irregular rhythm
- Absence of P waves
- Absence of an isoelectric baseline
- Variable ventricular rate
- QRS complexes < 120 ms
- How should the GP manage the patient?
Show Answer
In this case, the patient has a rate in excess of 150 bpm, therefore even in the absence of cardiovascular compromise or complications, the most appropriate course of action would be an urgent referral for hospital admission.
The current NICE guidance lists the following as indications for urgent referral for admission to hospital:
- There is a very rapid pulse (greater than 150 bpm) and/or low BP (systolic BP < 90 mm Hg)
- There is loss of consciousness, severe dizziness, ongoing chest pain, or increasing breathlessness
- There is a complication of AF (e.g. stroke, TIA or acute heart failure)

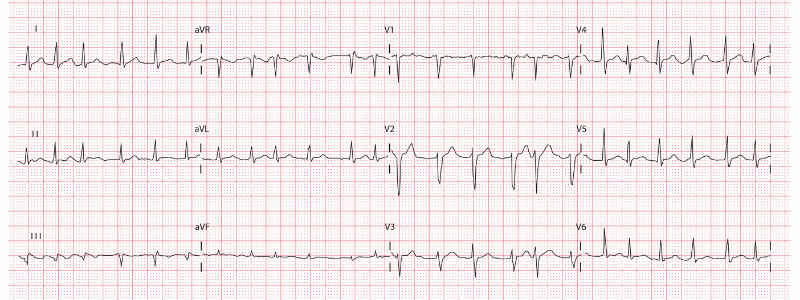




It is a good case to improve knowledge
good,useful
A very frequent Scenario in A & E I would Share with other Trainee in A & E