Osteoporosis causes no symptoms until a fragility fracture occurs and the mainstay of management is based upon preventing these fractures. Management should involve risk assessment, lifestyle advice and pharmacological treatment.
Lifestyle advice
Important lifestyle measures that can help to sustain bone mineral density and prevent fragility fractures include:
- Nutritional advice and optimisation
- Ensuring an adequate daily intake of calcium and vitamin D
- Emphasizing the importance of regular weight-bearing exercise
- Taking steps to reduce falls, e.g. removal of fall hazards in the home and muscle strengthening
- Reducing the risk of falls, e.g. wearing hip protectors
- Advice on smoking cessation
- Moderation of alcohol intake
- Avoidance of sedative drugs where possible
Elderly patients who are resident in a nursing home or are housebound can be assumed to be vitamin D deficient. If there is an adequate intake of dietary calcium (>1000 mg/day), but a deficiency vitamin D, consider prescribing 10 micrograms (400 units) of vitamin D without a full replacement dose of calcium. If there is an inadequate intake of calcium, then 1000 mg daily of calcium daily can be added (e.g. two Calcichew D3 tablets).
Pharmacological treatments
The pharmacological treatments used in the prevention of osteoporotic fragility fractures include:
- Oral and intravenous bisphosphonates
- Denosumab
- Raloxifene
- Teriparatide
First-line treatment for the primary prevention of fragility fractures
Oral bisphosphonates are the first-line treatment used in the primary prevention of osteoporotic fragility fractures. Choices include alendronic acid, ibandronic acid and risedronate sodium, but alendronic acid is often used on the basis of cost.
The current NICE guidance is that treatment with an oral bisphosphonate is indicated when a person eligible for risk assessment with an appropriate tool (FRAX or Qfracture) has a 10-year probability of osteoporotic fragility fracture of at least 1%.
Intravenous bisphosphonates can be used as an alternative if the 10-year probability of osteoporotic fragility fracture is at least 10%, or the 10-year probability is at least 1%, and the person has difficulty taking oral or these drugs are contraindicated or not tolerated.
The choice of treatment should be made on an individual basis after discussion between the prescribing clinician and the patient about the advantages and disadvantages of the available treatments.
Treatment with a bisphosphonate should continue for three years, but there is no evidence of ongoing benefit after this period. After three years of treatment, it is therefore recommended that a discussion should be held about discontinuing treatment.
Alternative primary prevention treatments
Denosumab is the main alternative treatments used in the primary prevention of fragility fractures. It is a human monoclonal antibody that inhibits osteoclast formation, function, and survival, thereby decreasing bone resorption.
Denosumab is recommended by NICE as an alternative treatment only in postmenopausal women at increased risk of fractures:
- Who are unable to comply with the special instructions for administering a bisphosphonate, or have an intolerance of, or a contraindication to a bisphosphonate, and;
- Who have a combination of T-score, age and number of independent clinical risk factors for fracture* as indicated in the following table:
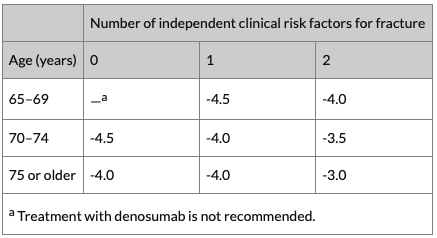
* Independent clinical risk factors for fracture are parental history of hip fracture, alcohol intake of 4 or more units per day, and rheumatoid arthritis.
Secondary prevention treatments
Oral bisphosphonates are the first-line treatment used in the secondary prevention of osteoporotic fragility fractures, i.e. in those who have suffered an osteoporotic fragility fracture. Following a fragility fracture it is recommended that a bisphosphonate is commenced (usually alendronic acid) and calcium and vitamin D supplementation should be considered.
Alternative treatment options for the secondary prevention of fragility fractures include:
- Raloxifene
- Teriparatide
- Denosumab
Raloxifene is a second-generation selective oestrogen receptor modulator (SERM) that reproduces the beneficial effects of oestrogens on the skeletal systems, without the negative effects oestrogens on breast and endometrium. It is recommended by NICE as an alternative treatment option for the secondary prevention of osteoporotic fragility fractures in postmenopausal women:
- Who are unable to comply with the special instructions for administering a bisphopshonate, or have an intolerance of, or a contraindication to a bisphosphate, and;
- Who also have a combination of T-score, age and number of independent clinical risk factors for fracture as indicated in the following table:
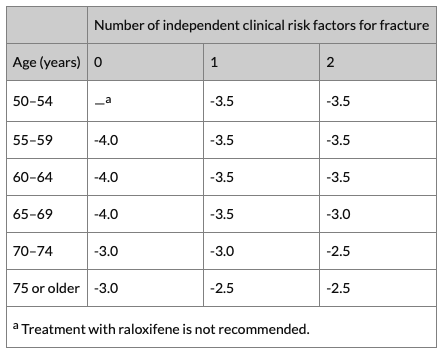
* Independent clinical risk factors for fracture are parental history of hip fracture, alcohol intake of 4 or more units per day, and rheumatoid arthritis.
Teriparatide is a recombinant protein form of parathyroid hormone. It is recommended by NICE as an alternative treatment option for the secondary prevention of osteoporotic fragility fractures in postmenopausal women:
- Who are unable to take, or are intolerant of, or who have had an unsatisfactory response to treatment with a bisphosphonate, and;
- Who are 65 years or older and have a T-score of -4.0 SD or below, or a T-score of -3.5 SD or below plus more than two fractures, or who are aged 55-64 years and have a T-score of -4 SD or below plus more than two fractures
Denosumab is recommended as a treatment option for the secondary prevention of osteoporotic fragility fractures only in postmenopausal women at increased risk of fractures who are unable to comply with the special instructions for administering a bisphosphonate or have an intolerance of, or a contraindication to, those treatments. Women currently receiving denosumab for the secondary prevention of osteoporotic fragility fractures who do not meet the criteria specified should have the option to continue treatment until they and their clinician consider it appropriate to stop.
Referral to secondary care
Referral to a secondary care metabolic bone clinic should be considered in the following situations:
- Diagnostic difficulty has occurred
- There has been an intolerance to oral bone-sparing therapy
- Continued fracture while on therapy
- Severe osteoporosis which may require specialised osteoporosis treatments, e.g. teriparatide therapy, strontium ranelate
- Other metabolic bone diseases such as osteomalacia or Paget’s disease
- Confirmed osteoporosis or low trauma fractures in men
Further reading:
NICE guideline: Osteoporosis: assessing the risk of fragility fracture
NICE Clinical Knowledge Summary: Osteoporosis
NICE technology appraisal guide: Bisphosphonates for treating osteoporosis
Header image used on licence from Shutterstock
Thank you to the joint editorial team of www.mrcgpexamprep.co.uk for this article.






