A 70-year-old woman presents with palpitations and breathlessness. Her observations show that she is hypotensive and tachycardiac, and she is complaining of chest pain. She is promptly transferred to resus. After being moved to resus she is administered three synchronized DC shocks, but her condition is unchanged. An ECG is taken following the shocks, which is shown below:
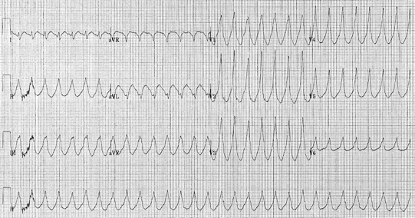
1. What does the rhythm strip show?
Show Answer
The rhythm shown in this case is clearly monomorphic ventricular tachycardia (VT). VT results from abnormal electrical signals in the ventricles causing the heart to beat faster than normal, usually >100 bpm and out of sync with the upper chambers. The QRS complexes are also typically very broad (>160 ms).
ECG sourced from Wikipedia
Courtesy of Dr. Karthik Sheka CC BY-SA 2.5
2. What is the likely physiological effect of this cardiac rhythm?
Show Answer
VT may impair cardiac output with consequent hypotension, collapse, and acute cardiac failure.
3. According to the ALS guidelines what should be the next management step?
Show Answer
The next step should be the administration of amiodarone 300 mg IV.
Synchronised DC shock in the peri-arrest setting is reserved for patients with any of the following four adverse features:
- Shock
- Syncope
- Myocardial ischaemia
- Heart failure
If the initial 3 shocks are unsuccessful, the ALS guidelines recommend the following treatment protocol:
- Seek expert help
- Give amiodarone 300 mg IV over 10-20 minutes
- Repeat shock
- Then give amiodarone 900 mg over 24 hours
Lidocaine can be used as an alternative, but amiodarone is the first-choice drug according to the current ALS guidelines.
Header image used on licence from Shutterstock