A 67-year-old woman presents to her local walk-in centre with a rash on her left forearm. She has a background of well-controlled hypertension, managed with amlodipine 5 mg once daily. She reports feeling well overall but mentions that her arm is slightly sore and that she has felt shivery over the past two days.
She recalls walking in a local park with friends one week ago and passing through an area of long grass. She thinks she may have seen a tick on her arm at the time.
On examination:
- She is apyrexial
- Blood pressure: 139/92 mmHg
- Heart rate: 88 bpm, regular
- Respiratory rate and oxygen saturation are normal
- Heart sounds are normal, and her chest is clear on auscultation
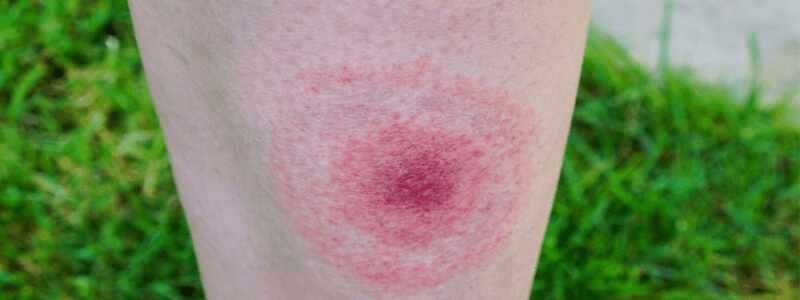
- Inspection of her left forearm reveals a ring-like erythematous rash with a central lesion.
Show Answer
The most likely diagnosis is early Lyme disease, caused by infection with Borrelia burgdorferi, a spirochete bacterium transmitted by Ixodes ticks.
The clinical history is highly suggestive: recent tick exposure in a grassy area, flu-like symptoms, and the appearance of a typical expanding rash are hallmark features.
Lyme disease is increasingly reported in the UK, particularly in spring and summer, and is endemic in many rural and even urban green spaces, including parks.
Transmission typically requires prolonged attachment of the tick (at least 16–24 hours), which is why prompt removal of ticks is key to prevention.
Show Answer
The rash is known as erythema migrans — the classical skin manifestation of early Lyme disease.
It usually develops 3 to 30 days after a tick bite. The rash often starts as a small red papule at the site of the bite and expands gradually, forming a ring-like lesion with central clearing. It may or may not be warm, painful, or itchy.
Diagnosis of Lyme disease in the presence of erythema migrans does not require laboratory confirmation — serological tests are often negative in early disease and are not necessary to start treatment.
3. How should this condition be managed?
Show Answer
In patients with uncomplicated erythema migrans, oral antibiotic therapy should be started promptly. Treatment options include:
- Doxycycline 100 mg twice daily for 21 days (first-line, unless contraindicated)
- Amoxicillin 500 mg three times daily for 21 days (preferred in pregnant or breastfeeding patients, or where doxycycline is unsuitable)
- Cefuroxime 500 mg twice daily for 21 days (alternative if both above are contraindicated)
Early treatment is effective and helps prevent progression to disseminated or late-stage disease.
Referral to an infectious diseases specialist should be considered if:
- There is diagnostic uncertainty
- The patient develops systemic or neurological symptoms
- The rash is atypical or persistent despite treatment
- There are concerns about treatment failure
Show Answer
If left untreated, Lyme disease can cause a wide range of multisystem complications. These include:
Neurological:
- Cranial nerve palsies (especially facial nerve – unilateral or bilateral)
- Meningitis or meningoencephalitis
- Radiculopathy (Bannwarth syndrome)
- Vertigo or peripheral neuropathy
Cardiac:
- Lyme carditis (can cause AV block, myopericarditis)
Musculoskeletal:
- Lyme arthritis — often affects large joints like the knees, and may be intermittent or chronic
Skin:
- Acrodermatitis chronica atrophicans (a late manifestation; causes bluish-red patches and skin thinning, typically on the extensor limbs)
General / Long-Term:
- Fatigue, myalgia, cognitive fog, or neuropsychiatric symptoms (post-treatment Lyme disease syndrome, sometimes loosely called “Post-Lyme syndrome”)
Teaching Points
✅ A clinical diagnosis of Lyme disease can be made in the presence of erythema migrans, even if serology is negative.
✅ Early treatment prevents complications — do not delay antibiotics while awaiting test results.
✅ Ticks are common not just in rural woodlands but also in urban parks and gardens.
✅ Public education on tick bite prevention and early recognition of symptoms is critical as Lyme disease incidence rises.
Header image used on licence from Shutterstock