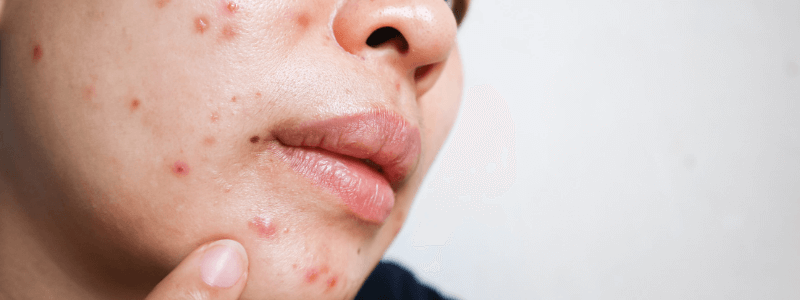
You review a patient with moderately severe acne that has been treated with a variety of topical agents over the past 6 months. There has been a poor response treatment and you consider switching to an oral antibiotic. You are aware that there is an increasing issue with antibiotic resistance in the management of acne.
- What is the most common pathogen implicated in the pathogenesis of acne?
Show Answer
Acne is a disorder affecting the pilosebaceous follicles found in the face and upper trunk. At puberty, androgens increase the production of sebum from enlarged sebaceous glands that become blocked.
The skin commensal bacterium Propionibacterium acnes is involved in the pathogenesis, but the exact mechanism is not fully understood.
- Which topical agent is recommended to be used in combination with oral antibiotics in the treatment of acne?
Show Answer
Antibiotic resistance is an increasing problem in the management of acne, and antibiotics are becoming less effective over time. Topical antibiotics are most affected, and the resistance rates to topical erythromycin and clindamycin in Propionibacterium acnes varies between 45-90%. It is recommended that topical benzoyl peroxide should be used in combination with a topical retinoid in preference to topical antibiotics to minimise the impact of bacterial resistance.
Oral antibiotics continue to be used in the treatment of moderate acne that has not responded to topical treatment. As with topical preparations, they should always be used in combination with topical benzoyl peroxide.
- What is the maximum time period that oral antibiotics should be used for in a single treatment for the management of acne?
Show Answer
Because of the problems with antibiotic resistance it is now advised that oral antibiotics should only be used for 3 months.
Header image used on licence from Shutterstock