Addison’s disease (primary adrenal insufficiency) is caused by the underproduction of the steroid hormones by the adrenal glands. Glucocorticoid, mineralocorticoid and sex steroid production are all affected. It is more common in women than in men and most commonly occurs between the ages of 30 and 50.
Aetiology
Autoimmune adrenalitis is the commonest cause of primary adrenal insufficiency, and this accounts for approximately 70-85% of cases.
Other causes include:
- Surgical removal of adrenal glands
- Trauma
- Infection, e.g. tuberculosis, HIV, cryptococcosis
- Infraction, e.g. antiphospholipid syndrome
- Haemorrhage, e.g. Waterhouse-Friderichsen syndrome
Clinical features
The clinical features of Addison’s disease tend to develop gradually and may become established before they are recognised. They can be non-specific and are sometimes attributed to other medical conditions before a definitive diagnosis is made.
The clinical features of Addison’s disease include the following:
- Weakness and lethargy
- Hypotension (notably orthostatic hypotension)
- Nausea and vomiting
- Weight loss
- Reduced axillary and pubic hair
- Depression
- Hyperpigmentation (palmar creases, buccal mucosa and exposed areas more commonly affected)
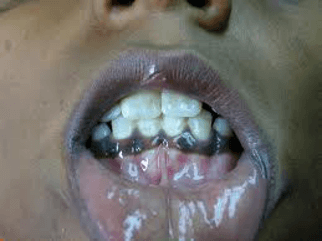
Hyperpigmentation in the oral mucosa of a patient with Addison’s disease
Investigations
In the early stages of Addison’s disease, investigations may be normal. The classical biochemical features of Addison’s disease are as follows:
- Hyponatraemia
- Hyperkalaemia
- Hypercalcaemia
- Hypoglycaemia
- Metabolic acidosis
Cortisol levels are usually reduced in Addison’s disease and can be measured with relative ease. Because of the pulsatile nature and diurnal variation of cortisol secretion, random cortisol measurements have a low sensitivity for diagnosis. Bloods should be taken between 8 am and 9 am for this reason when cortisol levels are at their highest. Cortisol results are unreliable in shift workers (due to disrupted diurnal variation), people taking oestrogen (can increase cortisol-binding globulin production by the liver), pregnancy, and in long-term corticosteroid usage. In these patient groups, specialist input from an endocrinologist is recommended.
Serum cortisol levels can be interpreted as follows:
- <100 nanomol/L – adrenal insufficiency very likely
- 100-400 nanomol/L – adrenal insufficiency possible and further investigations warranted
- >400 nanomol/L – adrenal insufficiency unlikely
ACTH levels, when measured in combination with cortisol levels, allow differentiation of primary from secondary adrenal insufficiency:
- Levels are raised in primary insufficiency
- Levels are low or low normal in secondary insufficiency.
Plasma renin and aldosterone levels can also be helpful; they are indicative of mineralocorticoid activity. In primary adrenal insufficiency renin levels are usually high and aldosterone levels low. Levels are usually unaffected in secondary insufficiency.
A Synacthen test may be required to confirm the diagnosis. ACTH is administered, either intravenously or intramuscularly, and cortisol levels subsequently measured. Under normal circumstances, a rise in the serum cortisol level would be expected. In adrenal insufficiency, this will not occur.
Associated conditions
Addison’s disease is associated with an increased incidence of the following conditions:
- Type I diabetes mellitus (not type II)
- Hashimoto’s thyroiditis
- Grave’s disease
- Premature ovarian failure
- Pernicious anaemia
- Vitiligo
- Alopecia
Management
Management should be by an Endocrinologist. Typically, patients require hydrocortisone, fludrocortisone and dehydroepiandrosterone. Some patients also require thyroxine if there is hypothalamic-pituitary disease present. Treatment is life-long, and patients should carry a steroid card and a MedicAlert bracelet and be aware of the possibility of an Addisonian crisis.
Addisonian Crisis
Addisonian crisis is a rare condition but can be catastrophic if the diagnosis is missed. In an Addisonian crisis, the main features are usually hypoglycaemia and shock (tachycardia, peripheral vasoconstriction, hypotension, altered conscious level, and coma). Other clinical features that can be present include:
- Fever
- Abdominal and leg pain
- Vomiting and dehydration
- Convulsions
- Psychosis
The initial management of an Addisonian crisis usually occurs in the Emergency Department setting and is as follows:
- Commence IV fluids, e.g. 20 ml/kg bolus of crystalloid
- Commence broad-spectrum antibiotics
- Treat hypoglycaemia with 50mls 50% IV dextrose
- Stat dose of IV hydrocortisone 100mg
- Take blood cultures, urine cultures and sputum for MC&S (preferably before the administration of IV antibiotics)
Header image used on licence from Shutterstock
Thank you to the joint editorial team of www.plabprep.co.uk for this ‘Exam Tips’ post.







Keep posting similar topics ,good for revision…………..