Non-invasive ventilation (NIV) is the administration of ventilatory support without the use of an invasive airway measure (e.g. endotracheal intubation or tracheostomy tube). It can be applied using a variety of devices including facemasks, nasal masks, various designs of mouthpiece, and specially designs helmets.
The use of NIV has become much more commonplace over the past 10-15 years, and it is used now used to treat respiratory failure in the Intensive Care Unit, the Emergency Department, on the wards, and even in patient’s homes.
What is Respiratory Failure?
Respiratory failure occurs when the respiratory system fails in either one or both of its gas exchange functions: oxygenation and the elimination of carbon dioxide. A reduction in the oxygen carried in the bloodstream is referred to as hypoxaemia, and a rise in the carbon dioxide levels within the bloodstream is referred to as hypercapnia.
Respiratory failure is classified into two groups:
- Type I respiratory failure
- Type II respiratory failure
Type I respiratory failure occurs when there is a problem with oxygenation resulting in hypoxaemia. This is most commonly caused by ventilation/perfusion mismatch resulting in reduced diffusion of oxygen from the alveoli into the pulmonary circulation. Type I respiratory failure is characterized by:
- Reduced PaO2 (< 8.0 kPa or 60 mmHg)
- Normal or reduced PaCO2 (< 6.7 kPa or 50 mmHg)
Type II respiratory failure occurs when there occurs when there is inadequate alveolar ventilation resulting in hypoxaemia and hypercapnia. Type II respiratory failure is characterized by:
- Reduced PaO2 (< 8.0 kPa or 60 mmHg)
- Elevated PaCO2 (> 6.7 kPa or 50 mmHg)
- Reduced pH (< 7.35)
Type II respiratory failure can be further sub-classified depending on the pre-existing condition of the patient and the speed of onset:
- Acute type II respiratory failure: the patient will have no, or minor, evidence of pre-existing respiratory disease and patients typically have a high PaCO2, low pH, and normal bicarbonate
- Chronic type II respiratory failure: evidence of chronic respiratory disease, high PaCO2, normal pH, and high bicarbonate.
- Acute-on-chronic type II respiratory failure: an acute deterioration in an individual with significant pre-existing type II respiratory failure, high PaCO2, low pH, and high bicarbonate.
Some of the more common causes of type I and type II respiratory failure are shown in the table below:
| Type I respiratory failure | Type II respiratory failure |
|---|---|
| Pneumonia Atelectasis Pulmonary embolism Acute pulmonary oedema High altitude Acute respiratory distress syndrome | Exacerbation of COPD Life-threatening asthma Obstructive sleep apnoea Extreme obesity Chest deformity e.g. kyphoscoliosis Cystic fibrosis Neuromuscular disorders |
Types of Non-Invasive Ventilation
Broadly speaking there are two main types of non-invasive ventilation:
- Continuous positive airway pressure (CPAP)
- Bilevel Positive Airway Pressure (BiPAP)
Continuous positive airway pressure (CPAP)
CPAP provides one single selected pressure throughout the entire respiratory cycle.
As the patient breathes in, this additional pressure recruits alveoli, increasing the surface area available for gas exchange to occur within and decreasing the patient’s work of breathing.
When the patient breathes out they will be doing so against the resistance of this continuous pressure. The recruited alveoli will therefore remain open at the end of expiration, increasing the functional residual capacity, resulting in more time being available for gas exchange to occur.
Bilevel Positive Airway Pressure (BiPAP)
BiPAP uses a time-cycled or flow-cycled change between two applied levels of positive airway pressure. One pressure is selected for inspiration (inspiratory positive airway pressure or ‘IPAP’), and one pressure is selected for expiration (expiratory positive airway pressure or ‘EPAP’).
The IPAP setting is set higher than the EPAP setting, providing the patient with the benefits of CPAP plus the additional benefit of increased support during inspiration. The higher IPAP pressure provides increased support as the patient breathes in, further reducing the patient’s work of breathing, and therefore respiratory muscle fatigue and myocardial oxygen demand. It also has the additional benefit of increasing the patient’s tidal volume, which helps to remove excess CO2 from the bloodstream.
As the EPAP setting is lower than the IPAP setting the patient will find it easier to breath out but the resistance of the pressure that is present in CPAP is still present. The benefit of the recruited alveoli remaining open at the end of expiration is therefore still present.
Pressure support is an important concept in BiPAP. It is equivalent to the difference between the inspiratory and expiratory pressures (i.e. pressure support = IPAP – EPAP). For example if the IPAP is set at 15 cmH2O and the EPAP at 10 cmH2O, then the pressure support is 5 cmH2O.
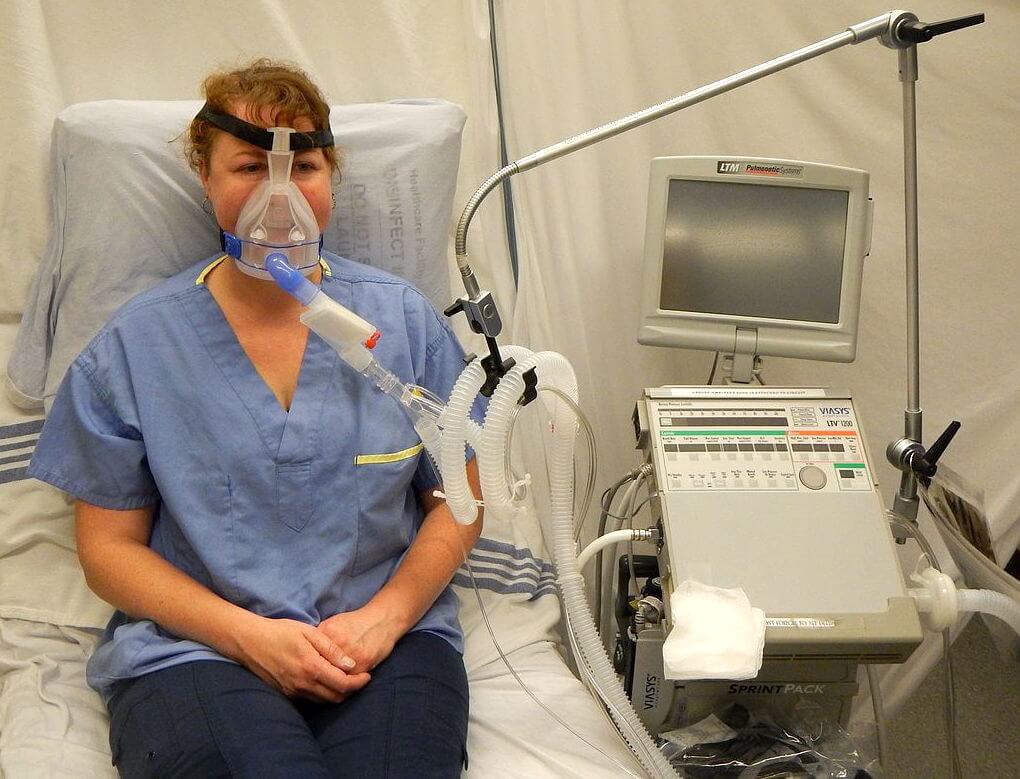
A typical BiPAP set up, image sourced from Wikipedia
Courtesy of Dr. James Heilman CC BY-SA 4.0
Initiating NIV
When initiating NIV it is very important to explain what is going to happen to the patient. Many people find the experience unpleasant and claustrophobic, but a thorough explanation and reassurance should help considerably. Make sure that the mask (or device of choice) fits well and that the straps are applied properly as a leak will significantly diminish the benefits.
An appropriate level of supplemental oxygen should be chosen and either a timed or flow cycled setting selected. It is advisable to start at low pressures, for example 5 cmH2O for CPAP and 10/5 cmH2O for BiPAP. If you are unsure which settings to use always seek advice from a senior, more experienced member of your team.
Generally speaking the pressures should be increased by 2-3 cmH2O every 5 minutes until a satisfactory response has been achieved. The pressure should usually not be set higher than 15-17 cmH2O.
Contraindications to NIV
The following are all absolute contraindications to the use of NIV:
- Respiratory arrest
- Cardiac arrest or unstable cardiorespiratory status
- Lack of patient consent or uncooperative patient
- Facial trauma or burns
- Reduced conscious level
- Untreated pneumothorax
- Base of skull fracture (due to risk of pneumocephalus)
- Intractable vomiting
- Absence of appropriately experienced staff
The following are considered to be relative contraindications to the use of NIV:
- Extreme patient anxiety
- Morbid obesity
- Copious secretions
- Lack of respiratory drive
Potential Complications of NIV
As with any treatment modality there are potential complications associated with the use of NIV that are important to be aware of. There are, however, fewer complications when compared with invasive ventilation.
The commonest complications associated with NIV are:
- Anxiety and/or claustrophobia (very common)
- Gastric distension and vomiting/aspiration
- Ulceration and pressure necrosis at the application site of the mask and straps
- Eye irritation
- Congestion of nasal sinuses
- Raised intracranial pressure
- Raised intraocular pressure
- Hypotension if hypovolaemia is present
Summary
Over recent years non-invasive ventilation has become an invaluable and flexible tool in the management of patients with respiratory failure. In many situations it has now replaced the need for invasive ventilation.
This article is not intended to be a comprehensive article covering all aspects of NIV, but hopefully should serve as a useful introduction to the topic and will encourage further reading and learning.
Thank you to the joint editorial team of www.mrcemexamprep.net for this article.
Header image used on licence from Shutterstock







It is very good effort regarding nimv ,hope same struggle ll b carried on
Regards
AWESOME .EXPLAINED NICELY FOR BEGINNERS.EXPECTING MORE TO COME.THANKS
This is straightforward to follow. And interesting.
Nіce рοst. I was ϲhecking continuously this blog and I am impressed!
Very useful info specificalⅼy the last part 🙂 I care
for such info a lot. I was seеking this certain info for a νery
long time. Thank yoᥙ and best of luck.