Hypothyroidism is a clinical syndrome that results from a deficiency of circulating thyroid hormones. It affects women more commonly than men and is most frequently seen in the over 60s.
The term myxoedema refers to a more severe form of the syndrome where there has been a deposition of mucinous substances resulting in thickening of the skin and subcutaneous tissues.
Aetiology
Hypothyroidism can be subclassified into:
- Primary hypothyroidism – the pathology affects the thyroid gland itself
- Secondary hypothyroidism – the thyroid gland is normal, but the production of stimulatory factors is abnormal.
Iodine deficiency is the most common cause of hypothyroidism worldwide.
The most common cause of hypothyroidism in the UK and other developed countries where iodine deficiency is not a problem is autoimmune thyroiditis. When this occurs in combination with a goiter, it is referred to as Hashimoto’s thyroiditis.
Clinical features
Hypothyroidism generally develops slowly over a period of months or years. The presentation can be very non-specific, particularly in the early stages of the disease.
The typical clinical features of hypothyroidism include:
- Tiredness and lethargy
- Cold sensitivity
- Dry skin
- Impaired concentration and memory
- Increased weight
- Decreased appetite
- Hoarse voice
- Reduced hearing/deafness
The typical ‘myxoedema facies’ seen in hypothyroidism are:
- Puffiness/oedematous facial appearance
- Dry skin
- Thinning of the hair
- Loss of the outer third of the eyebrows
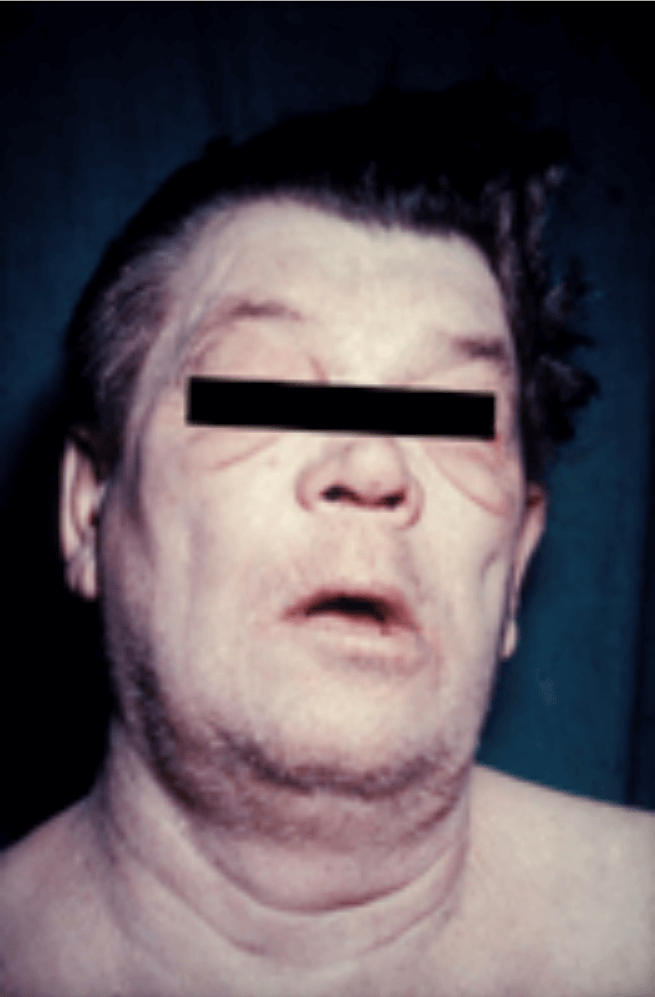
’Myxoedema facies’, image sourced from Wikipedia
Courtesy of Dr. L.F. Herbert et al. CC BY-SA 2.5
Investigations
Hypothyroidism is usually diagnosed based on of the results of thyroid function tests. Often in the early stages of the disease-free triiodothyronine (T3) and thyroxine (T4) levels are normal, and the earliest biochemical change that is noticed is generally a rise in thyroid-stimulating hormone (TSH) levels.
In overt primary hypothyroidism, the serum TSH level is usually greater than 10 mU/L, and free T4 levels are below the reference range.
Subclinical hypothyroidism can be diagnosed when the serum TSH level above the reference range, but the free T4 levels are within the reference range. In these circumstances, the test should be repeated after 3-6 months to exclude transient causes of raised TSH.
Secondary hypothyroidism is suggested by reduced free or total T4 with a TSH level below or within the normal range. If a diagnosis of secondary hypothyroidism is suspected, tests to evaluate hypothalamic and pituitary function should be requested.
Anti-thyroid peroxidase (anti-TPO) antibodies or anti-thyroglobulin antibodies are found in 90-95% of patients with autoimmune thyroiditis. NICE recommends measuring thyroid peroxidase antibodies (TPOAbs) for adults with TSH levels above the reference range, but not repeating TPOAbs testing.
A summary of how to interpret TFTs in cases of suspected hypothyroidism is shown in the table below:
| Diagnosis | TSH | Free T4 | Free T3 |
|---|---|---|---|
| Subclinical hypothyroidism | Raised | Normal | Normal |
| Primary hypothyroidism | Raised | Lowered | Lowered or normal |
| Secondary hypothyroidism | Lowered or normal | Lowered | Lowered or normal |
Management
The mainstay of treatment of overt hypothyroidism is with levothyroxine. Levothyroxine is usually started at a dose of 1.6 micrograms per kilogram of body weight per day (rounded to the nearest 25 micrograms) for adults under 65 with primary hypothyroidism and no history of cardiovascular disease (CVD). The usual maintenance dose is 100-200 micrograms once daily.
When a sufficient dose of thyroid treatment is given to lower the TSH to within the normal reference range, patients usually recover from the symptoms of hypothyroidism. It can, however, take many months and even up to six months after TSH levels have normalised for symptoms to resolve.
TSH should be measured every three months until the level has stabilised (two similar measurements within the reference range three months apart), and then once a year.
Header image used on licence from Shutterstock
Thank you to the joint editorial team of www.plabprep.co.uk for this article.







Thanks for your clear information 👍👍👍👍.
Really nice recap, thanks