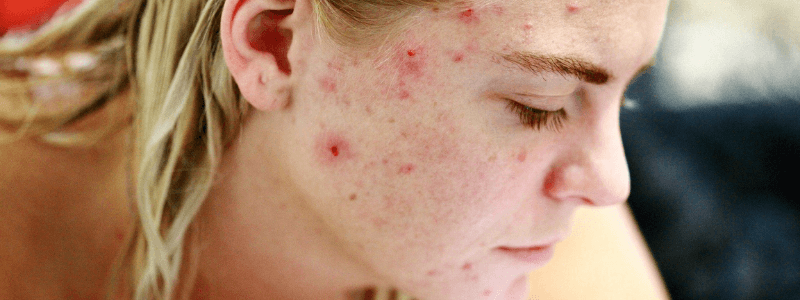
Acne vulgaris is a very common condition that affects children around the time of puberty. Virtually every teenager experiences a few ‘spots’, but approximately 15% will suffer acne of a severity that requires treatment. Acne seems like a trivial issue, but it can cause substantial distress, decreased self-confidence, and is associated with increased rates of depression and suicidal ideation.
Acne is a disorder affecting the pilosebaceous follicles found in the face and upper trunk. At puberty, androgens increase the production of sebum from enlarged sebaceous glands that become blocked. The skin commensal bacterium Propionibacterium acnes is involved in the pathogenesis, but the exact mechanism is not fully understood.
Possible triggers include:
- Increased levels of testosterone – e.g. occurring during puberty or in conditions such as PCOS.
- Family history
- Pregnancy
- Medications such as steroids and lithium
Clinical features of acne
Acne tends to affect areas of the body with a high density of pilosebaceous glands, namely:
- The face (most commonly affected area – 99% of cases)
- The back (60% of cases)
- The chest (15% of cases)
The clinical features vary widely depending on the severity and the person affected. Comedones must be present for a diagnosis of acne to be made, if there are no comedones present then alternate diagnoses should be considered.
The typical features of acne are as follows:
- Comedones – non-inflammatory lesions (which may be open (blackheads) or closed (whiteheads)
- Papules and pustules – superficial raised lesions (< 5 mm in diameter)
- Nodules or cysts – deeper, palpable lesions that are often painful and may be fluctuant. (> 5 mm in diameter)
- Seborrhoea – excessive discharge from the sebaceous glands is also commonly present
- Acne conglobata – a very severe form of acne where acne nodules track together and form sinuses
- Scarring – atrophic/ice pick or hypertrophic/keloid scars may be seen
- Pigmentation — post-inflammatory depigmentation or hyperpigmentation can occur.
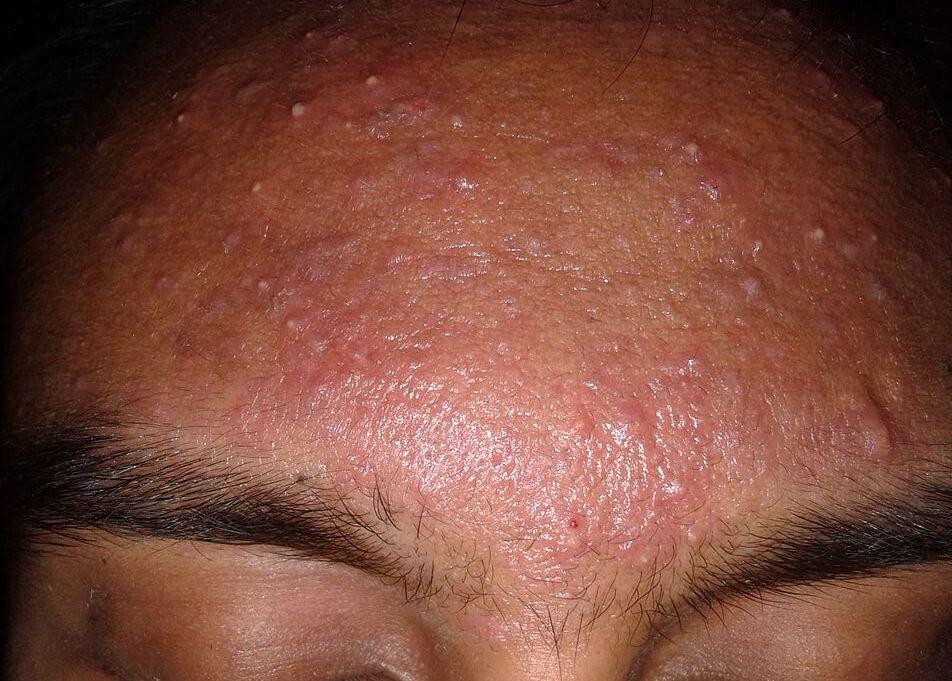
Moderately serve acne on the forehead of an 18-year-old male, image sourced from Wikipedia
Courtesy of Roshu Bangal CC BY-SA 4.0
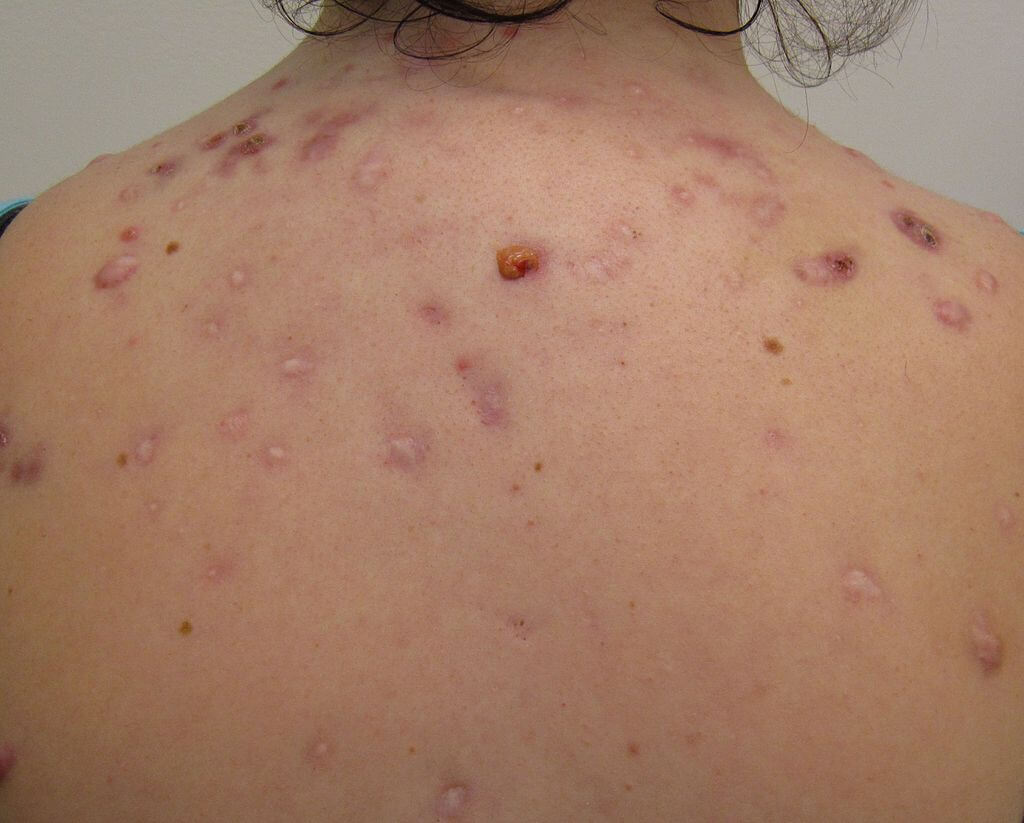
Nodular/cystic acne with scarring on the upper back, image sourced from Wikipedia
Courtesy of Dr. James Heilman CC BY-SA 3.0
Assessing acne severity
Acne can be categorised as mild, moderate and severe, which in turn is useful in the selection of appropriate treatment and monitoring of response:
- Mild acne – predominantly non-inflamed lesions (open and closed comedones) with few inflammatory lesions.
- Moderate acne – more widespread acne with an increased number of inflammatory papules and pustules.
- Severe acne – widespread inflammatory papules, pustules and nodules or cysts. Scarring may be present.
Management of acne
The primary aim of the treatment of acne is to prevent or at least minimise, scaring. The choice of treatment depends upon the severity of the acne, and a stepwise approach should be followed.
It is very important that all patients are educated about acne and the treatment options discussed appropriately. Self-care is of particular importance. The British Association of Dermatologists has a useful self-help leaflet that can be downloaded here.
Treatment of mild acne:
- Topical retinoids should be used first-line.
- Options include adapalene (Differin) and isotretinoin (Isotrex).
- Adapalene with 2.5% benzoyl peroxide (Epiduo gel) can also be used
- Topical retinoids should not be used in pregnancy.
- The second-line drug of choice is azelaic acid.
Treatment of moderate acne:
- Combination topical agents should be used, ideally containing benzoyl peroxide, which reduces bacterial resistance.
- First-line choice is adapalene with 2.5% benzoyl peroxide (Epiduo gel)
- Second-line choice is clindamycin with 2.5% benzoyl peroxide (Duac gel).
- Other options include clindamycin with tretinoin (Treclin gel) and erythromycin with tretinoin (Aknemycin).
Treatment of moderate acne not responding to topical treatment:
- A combination of systemic antibiotics with an appropriate topical agent should be used, preferably benzoyl peroxide, which reduces antibiotic resistance.
- First-line systemic antibiotic of choice is lymecycline 408 mg OD (Tetralysal).
- Review the patient at 6 weeks of treatment and switch to doxycycline 100 mg OD if the response is poor.
- Macrolides should generally be avoided due to high levels of Propionibacterium acnes resistance but can be used in pregnancy and in the under 12s, where tetracyclines are contraindicated.
- Trimethoprim can be used as a reserve option for children that are intolerant of erythromycin.
Treatment of severe acne:
- All patients with severe acne should be referred for specialist assessment and consideration of oral isotretinoin (Roaccutane)
- Treatment with a systemic antibiotic and an appropriate topical agent should be commenced in the interim period.
- Consider prescribing a combined hormonal contraceptive pill in women.
Antibiotic resistance in the treatment of acne
Antibiotic resistance is an increasing problem in the management of acne, and antibiotics are becoming less effective over time. Topical antibiotics are most affected, and the resistance rates to topical erythromycin and clindamycin in Propionibacterium acnes varies between 45-90%. It is recommended that topical benzoyl peroxide should be used in combination with a topical retinoid in preference to topical antibiotics to minimise the impact of bacterial resistance.
Oral antibiotics continue to be used in the treatment of moderate acne that has not responded to topical treatment. As with topical preparations, they should always be used in combination with topical benzoyl peroxide. Resistance to macrolides is particularly high, and these should be reserved for use only in children under 12 years of age and in pregnancy. It is now advised that oral antibiotics should only be used for 3 months.
Using combined hormonal contraceptives in the treatment of acne
The use of oral contraceptives as an alternative to oral antibiotics in women with moderate to severe acne where topical treatments have failed is recommended by several different guidelines.
The risks and benefits must be assessed on an individual basis — the combination of oestrogen with cyproterone and some other progestogenic hormones is associated with a 1.5-2 fold increased incidence of venous thromboembolism (VTE) compared with levonorgestrel-containing combined pills
Co-cyprindiol (Dianette) is licensed as a second-line treatment for women with severe acne when treatment with topical therapy or systemic antibiotics has failed.
The Faculty of Sexual and Reproductive Health guidance on Combined Hormonal Contraception has highlighted the increased risk of venous thromboembolism (VTE) associated with use of co-cyprindiol, and all women being prescribed it should be made aware of the increased risk of thrombosis compared to non-use or use of levonorgestrel-containing combined pills (1.5-2 fold increased incidence of VTE compared with levonorgestrel-containing combined pills). However, the absolute risk is still low if prescribed appropriately and is less than the risk associated with pregnancy, and the risks and benefits should be assessed on an individual basis
A meta-analysis of 32 randomized controlled trials found that although antibiotics may be superior at 3 months, combined oral contraceptives (COCPs) are equivalent to antibiotics at 6 months in reducing acne lesions
Referral from primary care for specialist assessment
Patients should be referred to a dermatologist for a specialist assessment if:
- They have a severe variant of acne, such acne conglobata
- They have severe acne associated with visible scarring or are at risk of scarring or significant hyperpigmentation
- Multiple treatments in primary care have failed
- Significant psychological distress is associated with acne regardless of severity
- There is diagnostic uncertainty.
Immediate referral is required for acne fulminans, a sudden severe inflammatory reaction that precipitates deep ulcerations and erosions, sometimes with systemic effects, such as fever and arthralgia.
Further reading:
NICE Clinical Knowledge Summary on the primary care management of acne
Stemming the tide of antimicrobial resistance: implications for the management of acne vulgaris
Thank you to the joint editorial team of www.mrcgpexamprep.co.uk for this ‘Exam Tips’ post.